Abstract
Introduction: Postpartum woman and child health is a public health concern as closely spaced pregnancies can lead to adverse maternal and infant outcomes. However, data regarding contraceptive intention among Malaysian postpartum women is lacking. Objective: This study aimed to determine the preferred contraceptive methods among postpartum women, the barriers to contraceptive use among non-users, and the willingness to seek contraceptive counselling provided by pharmacists, besides also aiming to explore factors associated with the intention to use contraceptives. Method: This research involved a cross-sectional study among postpartum women who delivered their babies in three main hospitals in Negeri Sembilan, Malaysia. A simple random sampling method was used to recruit study participants from September 2019 to January 2020. A face and content validated questionnaire was used for data collection. Descriptive data were presented as numbers and percentages. Pearson Chi-squared test and multiple logistic regression were used for inferential analysis. Result: The response rate was 98.8%. Of the 409 respondents, 84.8% were ≤ 35 years of age, 99.5% were married, and 79.2% were of Malay descent. More than half (62.9%) preferred using modern and non-modern contraceptive methods. The main barriers to contraceptive use were not feeling like using any contraceptive method (52%) and concerns about side effects (26.7%). Spouse education level (adj OR 2.141, 95% CI 1.267 – 3.617) and experience on previous formal contraceptive counselling (adj OR 3.642, 95% CI 2.091 – 6.343) significantly influenced the intention. The majority of respondents (82.4%) were willing to get contraceptive counselling from a pharmacist. Conclusion: The majority of the Malaysian postpartum women express interest in using both modern and non-modern contraceptive methods. Pharmacists could expand their services by advising on the appropriate choice of contraceptive methods in the future.
Introduction
Short interpregnancy interval is a public health concern. It is known that closely spaced pregnancies can lead to adverse maternal and infant outcomes, such as preterm birth [1][2][3], low birth weight [4][5][6], and small for gestational age [3]. In fact, the adverse pregnancy outcomes are higher for conceptions within the first-year postpartum [7], and can be further exacerbated if the pregnancy interval is less than six months [3,8]. The World Health Organization recommends a period of at least 24 months between a delivery and its pregnancy [9]. Indeed, by maintaining an interpregnancy interval of more than two years, greater than 30% of maternal deaths and 10% of child mortality could be prevented [10].
Because of the known harms, an adequately spaced pregnancy is of paramount importance. Unintended pregnancies after child delivery could be averted through postpartum contraception, also known as family planning, by initiating contraceptive methods within the first 12 months of delivery [11][12]. Generally, contraceptive methods, or birth control methods, can be categorised as modern and non-modern [13]. The effectiveness of each method varies across the board [14][15]. Data from low-to-middle-income countries have reported an overall pooled modern contraceptive prevalence rate of 41.2% during the postpartum period [16]. Meanwhile, in Malaysia, approximately 52.2% of married women aged between 15 – 49 have had prior use of, or were using family planning methods whereby 34.3% and 17.9% of women used modern and non-modern methods, respectively [13]. To date, however data on contraception among Malaysian postpartum women is still considerably lacking. Furthermore, the potential barriers to contraceptive use among local postpartum women have yet to be determined.
This study aimed to evaluate the intention of postpartum women to use contraception. The barriers faced by the participants against the use of contraceptives among non-users, and their willingness to obtain postpartum contraceptive counselling from a pharmacist were also assessed. The factors affecting contraceptive intention was also examined in the study.
Ethics approval
This study was registered with the National Medical Research Registry, Ministry of Health Malaysia (NMRR-19-363-45994). The questionnaire and methodology for this study were approved by The Medical Research and Ethics Committee, Ministry of Health Malaysia (KKM/NIHSEC/P19-1046).
Method
Study Design and Study Subjects
This was a multi-centred, cross-sectional study conducted in seven Obstetrics and Gynaecology (O & G) wards of three leading hospitals in Negeri Sembilan, Malaysia: Hospital Tuanku Ja’afar Seremban, Hospital Tuanku Ampuan Najihah, and Hospital Port Dickson from 1 September 2019 to 31 January 2020.
The target population was postpartum women hospitalised for at least one day at four O & G wards of Hospital Tuanku Ja’afar Seremban, two O & G wards of Hospital Tuanku Ampuan Najihah and one O & G ward of Hospital Port Dickson. Postpartum women who were ≥ 18 years old and understood the Malay or English language were included in the study. Patients who did not wish to be interviewed, were mentally and/or physically unstable, or did not complete the questionnaire were excluded.
There were 15 233 births in 2018, i.e., 10451 (~65%), 3588 (~25%), and 1194 (~10%) in Hospital Tuanku Ja’afar Seremban, Hospital Tuanku Ampuan Najihah, and Hospital Port Dickson, respectively. Preliminary considerations suggest that a total of 375 study subjects were needed after taking into account the number of births, a margin of error 5%, a confidence interval of 95%, and a response distribution of 52.2% [13]. Furthermore, it is suggested that approximately 450 postpartum women were required, with the presumption of 20% non-response rate. A total of 293 participants were patients from Hospital Tuanku Ja’afar Seremban, 113 from Hospital Tuanku Ampuan Najihah, and 45 from Hospital Port Dickson. Potential study subjects were recruited through a simple random sampling method by generating random numbers via Microsoft Office Excel. Written informed consent was obtained from study participants, and they had the right to withdraw from the study at any point during the study period.
Study instrument
A set of question for the questionnaire were written in the Malay and English languages and were used in this study. There were four main components in the questionnaire: sociodemographic background (Section A), the contraceptive intention (Section B), barriers to practice contraception (Section C), and willingness to get contraceptive counselling from the pharmacist (Section D). Section A included age, religion, participant’s highest education level, spouse’s highest
education level, employment status, household income, residence, duration of marriage, number of pregnancies, number of live births or children, experience of using contraceptive and formal contraceptive counselling. Section B encompassed contraceptive intention, methods preferred, reasons for using contraception and time to start contraception. The specific details related to modern and non-modern contraceptives were adapted from Mahmud, Jaffar, Hashim et al. (2014) [13] as well as Hubacher and Trussell (2015) [17]. The actual and potential barriers to practice contraception among non-users were documented in Section C [18], while Section D documented the willingness of postpartum women to receive contraceptive counselling from the pharmacist. The initial draft was reviewed by two senior pharmacy lecturers and five pharmacists with more than five years of working experience. The contents were revised accordingly and piloted among thirty postpartum women. Modifications were made for the second draft and piloted with another set of thirty postpartum women. Subsequently, the finalised questionnaire was distributed to the researchers for official data collection. The data obtained from the pilot tests were not included in the result.
Data collection
Before distributing the questionnaires to potential study subjects, the researchers would explain the study’s objectives and obtain written consent from the participants for participation in the study. Each study subject would take approximately 15 minutes to complete the questionnaire. The researchers would assist them in answering the questionnaire, where it is required.
Data analysis
Statistical analyse were performed using IBM® SPSS Statistics version 23.0. Categorical data were presented as numbers and percentages. The association between sociodemographic variables and the intention to use contraceptive was analysed with the Pearson’s Chi-squared test. Furthermore, all variables were included in the multiple logistic regression analysis to identify factors associated with contraceptive intention. A confidence interval of 95% was utilised in this study, and results were considered statistically significant if the two-tailed p-value was < 0.05.
Result
Socio-demography of respondents
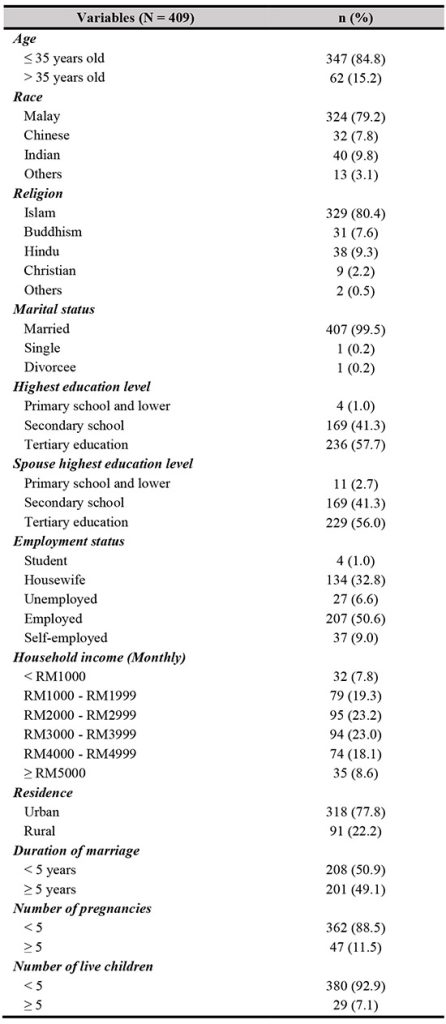
The response rate was 98.8% after excluding five incomplete questionnaires. Most of the respondents were ≤ 35 years old (n = 347, 84.8%), Malay (n = 324, 79.2%), of the religion of Islam (n = 329, 80.4%), married (n = 407, 99.5%), had received tertiary education (n = 229, 56%), employed (n = 207, 50.6%), from urban areas (n = 318, 77.8%), have had < 5 pregnancies (n = 362, 88.5%), and had < 5 live children (n = 380, 92.9%). Less than half of the respondents (n = 167, 40.8%) had some experience of using contraceptive prior to the current pregnancy. Approximately half of the respondents (n = 215, 52.6%) had received formal contraceptive counselling before the present childbirth. The sociodemographic characteristics of the 409 respondents are shown in Table I.
Contraceptive intention
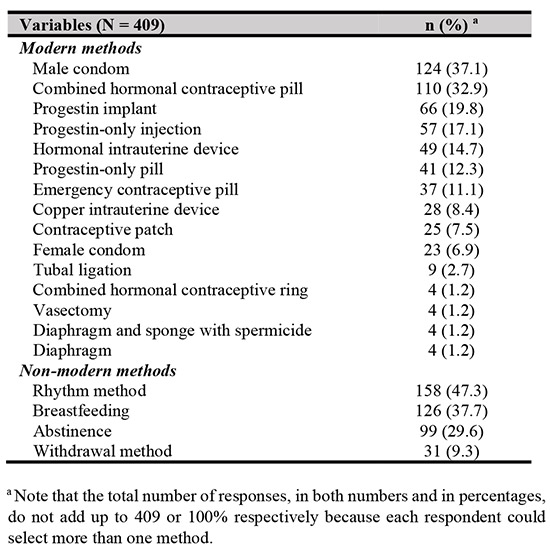
Most of the respondents (n = 334, 81.7%) had considered postpartum, of which 97 (29%), 27 (8.1%), and 210 (62.9%) considered modern methods, non-modern methods, and both methods respectively. Male condoms (n = 124, 37.1%), combined hormonal contraceptive pills (n = 110, 32.9%), progestin implants (n = 66, 19.8%) were among the modern contraceptive methods most favoured by the respondents. In contrast, combined hormonal contraceptive ring, vasectomy, diaphragm and sponge with spermicide, and diaphragm were among the less-preferred modern methods (for each of the four-method specified, n = 4, 1.2%). For non-modern contraceptive methods, the respondents preferred to use rhythm method (n = 158, 47.3%), followed by breastfeeding (n = 126, 37.7%), abstinence (n = 99, 29.6%), and the withdrawal method (n = 31, 9.3%). The details are summed up in Table II.
The reasons specified for the practices of postpartum contraception methods were also found to be as follow: to provide space (or a time gap) before attempting the next pregnancy (n = 245, 73.4%), to limit the number of children (n = 74, 22.2%), and others (n = 15, 4.5%).
Additionally, most respondents who chose to use contraception were unsure about the point in time on which such methods were to be initiated (n = 101, 30.2%). A total of 24% (n = 80) of participants were interested in beginning contraception six week postpartum, while the other participants specified initiation peroids between six weeks and six months postpartum (n = 58, 17.4%), between six months and one year postpartum (n = 45, 13.5%), after one year postpartum (n = 28, 8.4%), and before hospital discharge (n = 22, 6.6%).
Barriers to practise contraception
A total of 75 respondents who refused to use postpartum contraception for a number of reason, including the following:- not feeling like using contraception (n = 39, 52%), concerned about side effects (n = 20, 26.7%), husband’s disapproval (n = 6, 8%), complication during current pregnancy (n = 6, 8%), not expecting to have intercourse (n = 5, 6.7%), to have next child at short interval (n = 4, 5.3%), disturbance on sexual activities (n = 2, 2.7%), previous miscarriage (n = 2, 2.7%), lack of knowledge about contraceptive methods (n = 2, 2.7%), disturbance on social activities (n = 1, 1.3%), or other reasons (n = 1, 1.3%).

Willingness to receive pharmacist counselling
There were 337 (82.4%) study participants who were willing to seek out contraceptive counselling from a pharmacist in future. Only less than one fifth of the participants (n = 72, 17.6%) felt otherwise.
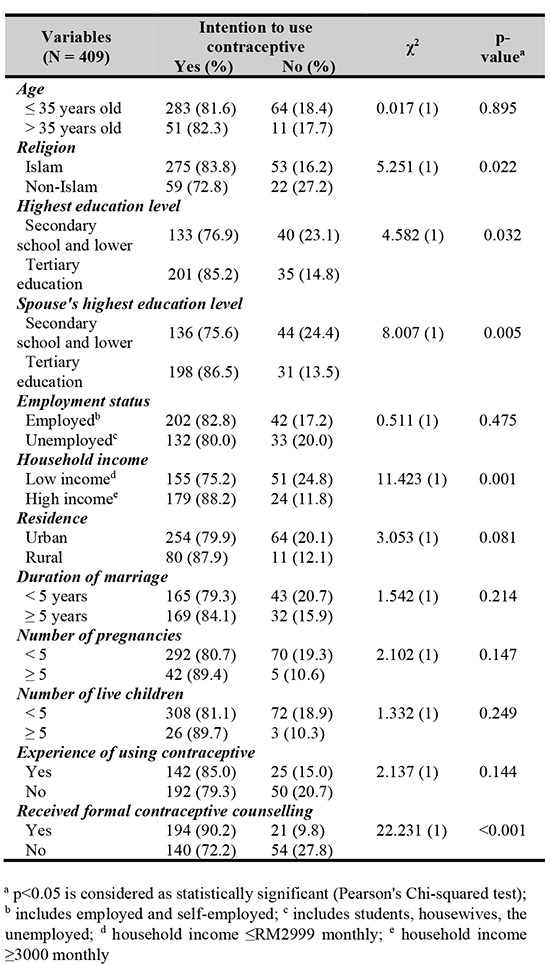
Association between sociodemographic characteristics and contraceptive intention
The association of respondents’ sociodemographic characteristics and their contraceptive intention were analysed using the Pearson’s Chi-squared test. The variables significantly associated with the intention were religion, respondent’s and spouse’s education level, household income, and experience of receiving formal contraceptive counselling (p < 0.05). There was no significant association between age, employment status, residence, duration of the marriage, number of pregnancies, number of live children, the experience of using contraception and the contraceptive intention. The details are shown in Table III.
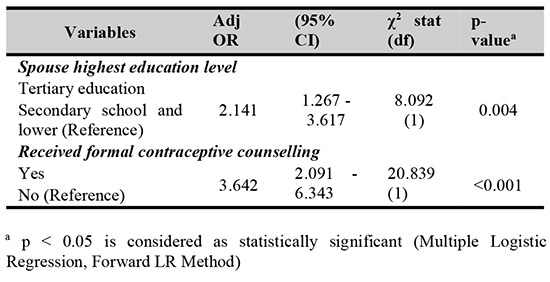
Multiple logistic regression suggested the spouse’s highest education level and experience of receiving formal contraceptive counselling before the current delivery significantly influenced a woman’s intention to use contraception. Postpartum women whose spouses had tertiary education were two times more likely to use contraception than those whose spouses had secondary or lower education (adj OR
2.141, 95% CI 1.267 – 3.617). Those who received formal contraceptive counselling were three times more likely to use contraception than their counterparts (adj OR 3.642, 95% CI 2.091 – 6.343). The details are presented in Table IV.
Discussion
There are various contraceptive methods available with different effectiveness and safety profiles. Irrespective of modern or non-modern methods, the first-year unintended pregnancy rate is low if used consistently and correctly [14].
In this study, preferred modern contraceptive methods include the use of male condom, followed by combined hormonal contraceptive pill and progestin implants. Meanwhile, the preferred non-modern method is the rhythm method, while other methods such as breastfeeding and abstinence follow suit, though they are relatively less used. These results are similar to a study conducted by Dev, Kohler, Feder, et al [16], whereby it is reported that injectables, oral contraceptive pills, condoms, breastfeeding, and rhythm methods are commonly used by postpartum women in low- and middle-income countries. Although similarity in preference can be observed, each contraceptive method’s uptake varies by country or region. For example, the uptake of injectables was only 2.7% in Nigeria [19] but could be as high as 68.5% in Ethiopia [20].
Breastfeeding is relatively common practice across different geographical borders. In fact, breastfeeding and rhythm methods are commonly used in West Africa [16], despite how breastfeeding was not found to be the first option of non-modern contraception in our study. The World Health Organization recommends mothers to exclusively breastfeed children for optimal growth, development, and health for the first six months [21]. Alongside these benefits are faster maternal weight loss after delivery and delayed return of menstrual periods postpartum [21]. However, as a contraceptive technique, it is noteworthy that breastfeeding is only effective for the first six months after childbirth and even if it used correctly, its effectiveness is known to be lower than other modern contraceptive options [14].
Furthermore, non-lactating women are potentially fertile because ovulation could occur as early as three to four weeks post-delivery [22], which can prove to be problematic as far as preventing pregnancies is concern, as sexual intercourse is believed to typically occur within the first six weeks postpartum [23,24]. This, therefore, further emphasises the importance of commencing contraception as early as possible during the postpartum period, in-line with the suggestion set by the World Health Organization to begin contraceptive methods
within the first 12 months following delivery [12]. Therefore to address this issue, timely counselling on contraceptive methods is essential to prevent unintended pregnancy.
Antenatal care services provide an opportunity to promote modern postpartum contraception due to their excellent utilisation [25][26]. Indeed, postnatal care services can further improved upon in order to match the extent of utilisation of antenatal care services, since the utilisation rates are comparatively lower than antenatal care service [26][27]. In support of this, Zapata, Murtaza, Whiteman, et al [28] reported on how the prevalence of postpartum contraceptive use was the highest when counselling was provided during both prenatal and postpartum periods. It is therefore crucial that the minimum interpregnancy interval and contraceptive choice should be emphasised during both antenatal and postnatal encounters to ensure that postpartum women understand the importance of contraception.
Emphasis should be placed on potential patient factors that may contribute to the use of contraceptives at each antenatal and postnatal encounter to ascertain an effective contraceptive counselling. Dev, Kohler, Feder, et al [16] reported that differences in the sociodemographic background could influence contraceptive practice among postpartum women. Specifically, women who were young, married, more educated, of higher socioeconomic status, and from urban residences, were more likely to use contraception [16]. Besides that, support from their male partners seems to be associated with contraceptive use during the postpartum period [16]. Findings from our study suggest that postpartum women whose spouses had tertiary education and those who received formal contraceptive counselling before the current delivery are more likely to practice contraception during the postpartum period. This supports the importance of proper counselling for both women and their spouses during antenatal care services to encourage postpartum contraceptive acceptance.
The reluctance of women to practice contraception or family planning can be attributed to a myriad of factors. Fear of adverse effects is a common cause for poor acceptance and high rates of contraception discontinuation among postpartum women [16], indicating that well-planned and intensified counselling sessions should be an integral part of antenatal and postnatal visits to encourage postpartum family planning. The adverse effects of contraceptive methods should be explained and appropriately addressed during these encounters to mitigate their worries, to allow them to understand options available to them, and receive advice on contraception methods that suits their needs. While doctors and nurses have been delivering antenatal and postnatal care services at present, pharmacists could expand their role in this service which requires multidisciplinary engagement. Unfortunately, literature findings on the impact of postpartum contraceptive counselling by pharmacists are scarce. Schatz, Chapman, and Chang [29] reported more than two-thirds of postpartum women would like to receive contraceptive counselling by a pharmacist, especially on hormonal and implantable forms of contraception. In this context, inpatient and clinical pharmacists are in a strategic position to provide contraceptive counselling for postpartum women. In addition to explaining contraceptive methods, a pharmacist can advise on patient-specific alternatives by examining their co-morbidities, potential drug-drug or drug-disease interactions, financial affordability, personal preferences, and others.
There are several limitations in this study. Although most of the study participants expressed desire to use contraception after childbirth, the prevalence of its practice among postpartum women is not confirmed during the postnatal care service. We also acknowledge the possibility of acquiescence bias, since study participants answered the questionnaire in the presence of researchers. Furthermore, the fact that this study was conducted in government-funded hospitals may implicate that the results may not be representative of patients in private healthcare facilities. Future research could be designed to check on the contraceptive prevalence rates among postpartum women, and to establish a causal relationship between factors affecting contraceptive use among women in this population.
Conclusion
The majority of postpartum women in this study expressed interest in using both modern and non-modern contraceptive methods. It was found that the main barriers to contraceptive use were inherent hesitancy to use any method and concerns about side effects. Fortunately, the majority of postpartum women were interested into receiving contraceptive counselling from a pharmacist. This study reports that the education level of spouses and prior formal counselling before child delivery of postpartum women significantly affect their contraceptive intention. Healthcare professionals, including pharmacists, could improve maternal and foetal health outcomes by providing contraceptive counselling, and by addressing effectiveness and side effects of postpartum contraceptives.
Acknowledgement
We would like to thank the Director General of Health, Malaysia for his permission to publish this article.
Conflict of Interest
This study has no conflict of interest. This research did not receive any specific grant from funding agencies in public, commercial or not-for-profit sectors.
Reference
- DeFranco EA, Stamilio DM, Boslaugh SE, Gross GA, Muglia LJ. A short interpregnancy interval is a risk factor for preterm birth and its recurrence. Am J Obstet Gynecol. 2007 Sep;197(3):264.e1-6. https://doi.org/10.1016/j.ajog.2007.06.042
- Fuentes-Afflick E, Hessol NA. Interpregnancy interval and the risk of premature infants. Obstet Gynecol. 2000 Mar;95(3):383-90. https://doi.org/10.1016/s0029-7844(99)00583-9
- Shults RA, Arndt V, Olshan AF, Martin CF, Royce RA. Effects of short interpregnancy intervals on small-for-gestational age and preterm births. Epidemiology. 1999 May;10(3):250-4. https://journals.lww.com/epidem/pages/articleviewer.aspx?year=1999&issue=05000&article=00010&type=abstract
- Khoshnood B, Lee KS, Wall S, Hsieh HL, Mittendorf R. Short interpregnancy intervals and the risk of adverse birth outcomes among five racial/ethnic groups in the United States. Am J Epidemiol. 1998 Oct 15;148(8):798-805. https://doi.org/10.1093/oxfordjournals.aje.a009701
- Zhu BP, Rolfs RT, Nangle BE, Horan JM. Effect of the interval between pregnancies on perinatal outcomes. N Engl J Med. 1999 Feb 25;340(8):589-94. https://doi.org/10.1056/NEJM199902253400801
- Zhu BP, Haines KM, Le T, McGrath-Miller K, Boulton ML. Effect of the interval between pregnancies on perinatal outcomes among white and black women. Am J Obstet Gynecol. 2001 Dec;185(6):1403-10. https://doi.org/10.1067/mob.2001.118307
- DaVanzo J, Hale L, Razzaque A, Rahman M. Effects of interpregnancy interval and outcome of the preceding pregnancy on pregnancy outcomes in Matlab, Bangladesh. BJOG. 2007 Sep;114(9):1079-87. https://doi.org/10.1111/j.1471-0528.2007.01338.x
- Conde-Agudelo A, Rosas-Bermúdez A, Kafury-Goeta AC. Birth spacing and risk of adverse perinatal outcomes: a meta-analysis. JAMA. 2006 Apr 19;295(15):1809-23. https://doi.org/10.1001/jama.295.15.1809
- World Health Organization, 2007. Report of a WHO technical,consultation on birth spacing: Geneva, Switzerland 13-15 June 2005,(No. WHO/RHR/07.1). World Health Organization,https://www.who.int/publications/i/item/WHO-RHR-07.1
- Cleland J, Bernstein S, Ezeh A, Faundes A, Glasier A, Innis J. Family planning: the unfinished agenda. Lancet. 2006 Nov 18;368(9549):1810-27. https://doi.org/10.1016/S0140-6736(06)69480-4
- World Health Organization: Programming strategies for postpartum,family planning. Geneva: World Health Organization. 2013,https://www.who.int/publications/i/item/9789241506496
- World Health Organization: Postpartum family planning: essential for ensuring health of women and their babies. World Contraception Day 2018.
- Mahmud A, Jaffar W, Hashim W, et al. Report on key findings Fifth Malaysian Population and Family survey (MPFS-5). 2014. https://www.researchgate.net/publication/321069633
- Trussell J and Aiken ARA, Contraceptive efficacy. In: Hatcher RA, Nelson AL, Trussell J, Cwiak C, Cason P, Policar MS, Edelman A, Aiken ARA, Marrazzo J, Kowal D, eds. Contraceptive Technology, 21st revised edition. New York, Ardent Media, 2018.
- Peragallo Urrutia R, Polis CB, Jensen ET, Greene ME, Kennedy E, Stanford JB. Effectiveness of Fertility Awareness-Based Methods for Pregnancy Prevention: A Systematic Review. Obstet Gynecol. 2018 Sep;132(3):591-604. https://doi.org/10.1097/AOG.0000000000002784. Erratum in: Obstet Gynecol. 2019 Feb;133(2):382.
- Dev R, Kohler P, Feder M, Unger JA, Woods NF, Drake AL. A systematic review and meta-analysis of postpartum contraceptive use among women in low- and middle-income countries. Reprod Health. 2019 Oct 29;16(1):154. https://doi.org/10.1186/s12978-019-0824-4
- Hubacher D, Trussell J. A definition of modern contraceptive methods. Contraception. 2015 Nov;92(5):420-1. https://doi.org/10.1016/j.contraception.2015.08.008
- Najimudeen M, Sachchithanantham K. An insight into low contraceptive prevalence in Malaysia and its probable consequences. Int J Reprod Contracept Obstet Gynecol. 2014;3(3):493-6. https://www.ijrcog.org/index.php/ijrcog/article/view/979
- Adeyemi AB, Ijadunola KT, Orji EO, Kuti O, Alabi MM. The unmet need for contraception among Nigerian women in the first year post-partum. Eur J Contracept Reprod Health Care. 2005 Dec;10(4):229-34. https://doi.org/10.1080/13625180500279763
- Abera Y, Mengesha ZB, Tessema GA. Postpartum contraceptive use in Gondar town, Northwest Ethiopia: a community based cross-sectional study. BMC Womens Health. 2015;15:19. https://doi.org/10.1186/s12905-015-0178-1
- World Health Organization. Exclusive breastfeeding for six months best for babies everywhere. 2011.https://www.who.int/news/item/15-01-2011-exclusive-breastfeeding-for-six-months-best-for-babies-everywhere
- Jackson E, Glasier A. Return of ovulation and menses in postpartum nonlactating women: a systematic review. Obstet Gynecol. 2011 Mar;117(3):657-662. https://doi.org/10.1097/AOG.0b013e31820ce18c
- Byrd JE, Hyde JS, DeLamater JD, Plant EA. Sexuality during pregnancy and the year postpartum. J Fam Pract. 1998 Oct;47(4):305-8. http://www.jstor.org/stable/3813687
- Rogers RG, Borders N, Leeman LM, Albers LL. Does spontaneous genital tract trauma impact postpartum sexual function? J Midwifery Womens Health. 2009 Mar-Apr;54(2):98-103. https://doi.org/10.1016/j.jmwh.2008.09.001
- Do M, Hotchkiss D. Relationships between antenatal and postnatal care and post-partum modern contraceptive use: evidence from population surveys in Kenya and Zambia. BMC Health Serv Res. 2013 Jan 4;13:6. https://doi.org/10.1186/1472-6963-13-6
- Regassa N. Antenatal and postnatal care service utilization in southern Ethiopia: a population-based study. Afr Health Sci. 2011 Sep;11(3):390-7. https://www.ajol.info/index.php/ahs/article/view/73402
- Sonalkar S, Hunter T, Gurney EP, McAllister A, Schreiber CA. A Decision Analysis Model of 1-Year Effectiveness of Intended Postplacental Compared With Intended Delayed Postpartum Intrauterine Device Insertion. Obstet Gynecol. 2018 Nov;132(5):1211-1221. https://doi.org/10.1097/AOG.0000000000002926
- Zapata LB, Murtaza S, Whiteman MK, Jamieson DJ, Robbins CL, Marchbanks PA, D’Angelo DV, Curtis KM. Contraceptive counseling and postpartum contraceptive use. Am J Obstet Gynecol. 2015 Feb;212(2):171.e1-8. https://doi.org/10.1016/j.ajog.2014.07.059
- Schatz K, Chapman J, Chang J. Examining the impact of a pharmacists postpartum counseling service; evidence from a university hospital. Innov Pharm. 2014 1 January;5(1). https://doi.org/10.24926/iip.v5i1.328
Please cite this article as:
Boon-Tiang Lau, Siew-Yen Ng, Mohd-Farizh Che-Pa, Muhammad-Faizal Maarof, Dinesh-Kumar Subaramaniam, Zetty-Ellyssa Sallehuddin, Noor-Izzati-Filza Salihoudin, Noor Husna Nazirah A Razak, Jing-Sze Teen, Kalai-Divvya Ramasamy and Syamimi-Aqilah Abdull-Kahar, Contraceptive Intention among Postpartum Women and Willingness for Pharmacist Counselling in Negeri Sembilan, Malaysia: A Cross-Sectional Study. Malaysian Journal of Pharmacy (MJP). 2022;1(8):19-25. https://mjpharm.org/contraceptive-intention-among-postpartum-women-and-willingness-for-pharmacist-counselling-in-negeri-sembilan-malaysia-a-cross-sectional-study/